Introduction: Why Hands-On Medicine Draws Attention
Many people search for care that looks beyond isolated symptoms. They want treatment that connects pain, posture, movement, and daily habits into one picture. Hands-on medicine answers that call. It blends anatomy knowledge with careful touch, aiming to support the body’s own capacity for balance and repair.
This article explains osteopathic manipulation therapy in clear terms. It covers where it came from, how it works, what a session feels like, and who often finds value in it. You will also read examples, expert perspectives, and practical guidance for patients new to this form of care.
The Roots of Osteopathic Care
Osteopathic medicine began in the late 1800s with Dr. Andrew Taylor Still, an American physician. He observed that structure and function of the body stay closely linked. When bones, muscles, and joints move freely, blood flow and nerve signals travel with less resistance.
Dr. Still believed hands could both diagnose and treat physical problems. This belief shaped a medical philosophy centered on touch, movement, and respect for the body as an integrated unit. Over time, osteopathic medicine grew into a regulated medical field taught at accredited schools.
What Osteopathic Manipulation Therapy Means
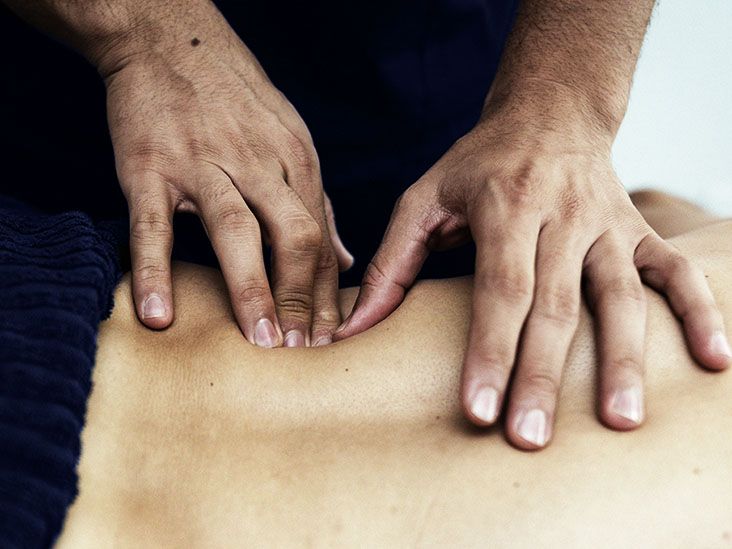
Osteopathic manipulation therapy, often shortened to OMT, uses manual techniques to improve motion and ease strain. A trained clinician applies gentle pressure, stretching, or guided resistance. Each technique matches the patient’s condition and comfort level.
The word “manipulation” sometimes causes concern. In this setting, it does not imply forceful action. Many techniques feel subtle and calm. The goal stays focused on restoring normal movement patterns.
Common Techniques Explained
OMT includes a wide range of approaches. Here are several often used methods:
- Soft tissue work: Slow stretching of muscles and connective tissue
- Myofascial release: Gentle pressure to reduce tension in fascia, the body’s connective web
- Muscle energy: Patient moves against light resistance from the practitioner
- Counterstrain: Positioning the body to reduce pain signals
- Joint articulation: Repetitive, low-force movement of joints
Each method targets a different layer of the musculoskeletal system.
How a Session Usually Unfolds
A typical visit begins with a conversation. The clinician asks about pain, daily activities, sleep, stress, and past injuries. This information guides the physical exam.
Next comes hands-on assessment. The practitioner checks posture, range of motion, and tissue texture. Areas of tightness or restricted movement stand out through touch.
Treatment follows assessment. Patients stay clothed and lie on a padded table. Techniques change based on findings and patient feedback. Many people notice warmth, relaxation, or a sense of release as the session continues.
Conditions Often Addressed
OMT does not focus on one diagnosis alone. It looks at movement patterns that contribute to discomfort. People seek this care for many reasons.
| Area of Concern | Examples |
|---|---|
| Spine and posture | Back pain, neck stiffness, uneven shoulders |
| Head and jaw | Tension headaches, jaw tightness |
| Limbs | Shoulder strain, hip discomfort, knee issues |
| Daily stress effects | Muscle tension, fatigue |
| Recovery support | Post-injury stiffness, limited motion |
Research published in journals such as The Journal of the American Osteopathic Association reports positive outcomes for low back pain, with reduced pain scores and improved function after OMT sessions.
A Practical Example: Office-Related Back Pain
Imagine a person who works long hours at a desk. Over time, shoulders round forward and the neck juts ahead. Back pain sets in, and stretching at home brings little change.
During an osteopathic visit, the clinician notices limited movement in the upper spine and tight chest muscles. Treatment focuses on soft tissue work across the shoulders and gentle articulation of the thoracic spine. Muscle energy techniques help retrain posture.
After several visits, the patient reports easier movement and less end-of-day discomfort. The clinician also shares simple posture habits for daily work life.
How OMT Differs From Other Manual Therapies
People often ask how OMT compares with chiropractic care or massage therapy. The table below outlines broad distinctions.
| Feature | OMT | Chiropractic Care | Massage Therapy |
|---|---|---|---|
| Training background | Medical education with osteopathic focus | Chiropractic education | Massage certification |
| Scope | Whole-body assessment | Spine-centered focus | Muscle relaxation |
| Techniques | Wide range, gentle to firm | Often high-velocity adjustments | Soft tissue manipulation |
| Medical integration | Full medical context | Musculoskeletal focus | Wellness support |
Each approach serves a purpose. OMT stands out for its integration with medical diagnosis and patient history.
Safety and Comfort
Safety remains central to osteopathic care. Techniques stay adapted to age, health status, and personal comfort. Practitioners receive extensive training in anatomy and hands-on evaluation.
Studies note low rates of adverse effects, most often mild soreness similar to post-exercise feelings. Communication during sessions allows adjustments at any time.
What Experts Say
Dr. Jane Smith, DO, wrote in a 2021 review that manual treatment “supports musculoskeletal balance while respecting the body’s self-regulating nature.” Her words echo a long-standing osteopathic principle.
The American Osteopathic Association also highlights research showing OMT’s role in pain management without reliance on medication. This point draws interest as people search for non-drug options.
Learning More and Exploring Options
Readers who want deeper information often look for educational resources that explain techniques and patient experiences. One example appears within the phrase osteopathic manipulation therapy St George, which offers an overview of concepts and care principles in plain language.
Exploring such material can help people prepare thoughtful questions before their first visit.
How to Prepare for a First Visit
Preparation helps patients feel at ease. Simple steps include:
- Wear comfortable clothing
- Bring notes about pain patterns or injuries
- Share goals, such as improved movement or reduced tension
- Stay open about comfort levels during treatment
Open communication builds trust and guides effective care.
Closing Thoughts: A Broader View of Movement and Health
Osteopathic manipulation therapy centers on the idea that the body works as a connected whole. Through skilled touch, practitioners aim to restore motion, ease strain, and support natural balance. History, research, and patient stories all point to its role in modern care.
For readers curious about hands-on approaches, learning the basics marks a helpful first step. From understanding techniques to knowing what a session feels like, knowledge builds confidence and clarity.